Scott Weidenfeller discusses medical malpractice related to failure to timely diagnose and treat oxygenation problems during labor and delivery – and during the neonatal period.
We see many cases in which healthcare providers fail to promptly diagnose and treat problems that cause reduced oxygenation in babies, which can cause or worsen a condition called hypoxic ischemic encephalopathy (HIE). In this term, hypoxic refers to oxygen deprivation in brain tissue, ischemic refers to reduced blood flow to brain tissue, and encephalopathy means brain disorder.
OXYGEN DEPRIVATION DURING OR NEAR THE TIME OF BIRTH
HIE can be caused by a delayed delivery when a baby is experiencing oxygen deprivation during or near the time of birth. Oxygen deprivation near the time of delivery can be caused by conditions such as a prolapsed umbilical cord, the umbilical cord being wrapped around the baby’s neck (nuchal cord), placental abruption, uterine rupture and really high or really low blood pressure in the mother. When a baby is experiencing oxygen deprivation in the womb, the fetal heart tracings will be abnormal or non-reassuring.
Signs that your baby may have experienced significant oxygen deprivation during or near the time of birth include the following:
- Your baby had low Apgar scores
- Your baby didn’t cry at birth and/or had a dusky or blue-ish color
- Your baby needed resuscitation
- Your baby had an umbilical cord blood gas that showed acidosis
- Your baby needed care in the ICU
- Your baby required hypothermia “brain cooling” treatment.
When a baby is deprived of oxygen near the time of delivery, she may sustain a brain injury, which can result in hypoxic ischemic encephalopathy (HIE).
Newborn babies who have HIE may experience breathing problems during the neonatal period, and it is important that these problems be promptly treated to prevent further brain injury.
OXYGEN DEPRIVATION DURING THE NEONATAL PERIOD
Breathing problems during the neonatal period can be caused by a wide variety of conditions. Premature babies have underdeveloped lungs, and thus, they may have problems that include respiratory distress syndrome and apnea of prematurity. Sometimes, babies that suffered an oxygen-depriving insult during or near the time of birth may continue to have breathing problems in the neonatal period. Many conditions can cause these post-birth breathing problems, one of which is meconium aspiration (the baby had a stool in utero and inhaled amniotic fluid that contains this stool).
Then there are babies who have congenital or physiological problems that impact oxygenation. One such physiological problem is called
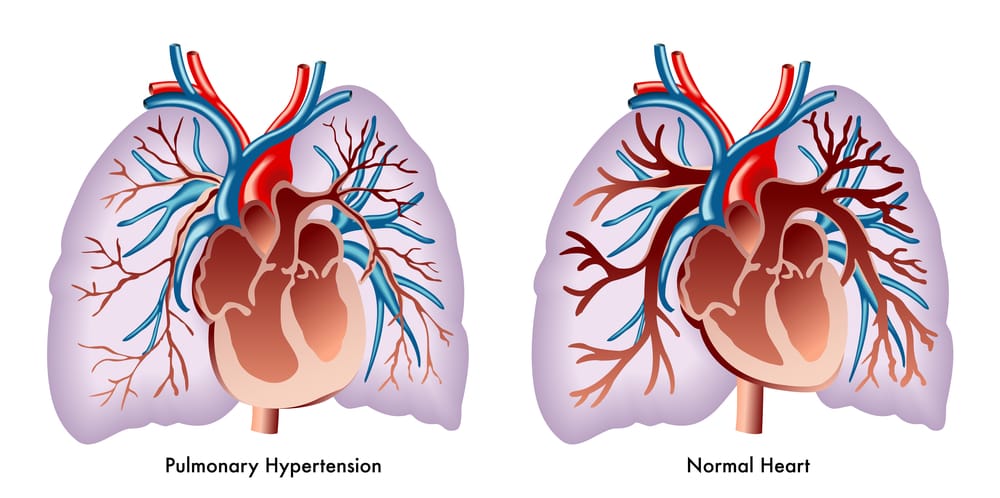
persistent pulmonary hypertension (PPHN), and this is a very serious condition in which the lung vessels of newborns are not open wide enough, which causes very high pressure in these vessels, which leads to a reduced oxygen level in the baby’s blood. If PPHN is not promptly diagnosed and treated, the baby can suffer permanent brain damage due to lack of oxygen. We recently had a case whereby the baby suffered a brain injury due to a delayed emergency C-section when he was experiencing hypoxia and fetal distress during the process of labor. Once the baby was born, he had clear signs of PPHN, such as low oxygen levels in his blood despite being given a lot of supplemental oxygen. Sadly, the healthcare team failed to recognize this very serious problem for days, and the child suffered additional brain injury that resulted in him having lifelong problems such as severe cerebral palsy, a seizure disorder and intellectual disabilities.
Physiological and congenital problems in newborns that require prompt diagnosis and treatment include the following:
- Persistent pulmonary hypertension (PPHN)
- Coarctation of the aorta (COA)
- Patent ductus arteriosus (also called PDA)
- Atrial septal defect (also called ASD)
- Ventricular septal defect (also called VSD)
- Atrioventricular septal defect (AVSD)
- Dextro-Transposition of the Great Arteries (also called d-TGA)
- Pulmonary atresia (also called PA)
- Ebstein anomaly
- Hypoplastic left heart syndrome (also called HLHS)
- Tricuspid atresia
- Tricuspid atresia
- Tetralogy of Fallot (also called TOF)
- Total anomalous pulmonary venous return (also called TAPVR)
- Truncus arteriosus (also called common truncus).
The above mentioned cardiac and pulmonary problems affect blood flow, and if these issues are not corrected, the lack of oxygen (which is caused by reduced blood flow) can cause damage to vital organs, including the brain. Some of the problems listed above will correct themselves on their own, but it is important that the healthcare team provide crucial supportive care while waiting to see if the congenital / physiological problems will become corrected. Other problems require urgent or emergent surgery and other treatments.
SIGNS THAT A BABY IS EXPERIENCING OXYGEN DEPRIVATION AND/OR IMPENDING RESPIRATORY FAILURE
Whatever the cause of a baby’s oxygenation problems or work of breathing issues (which can lead to respiratory failure, if not timely treated), prompt diagnosis and treatment is crucial in order to prevent the baby from suffering significant oxygen deprivation.
Below are some signs that a baby is experiencing oxygen deprivation:
- The skin is blue or dusky
- The baby seems lethargic
- The baby has abnormal vital signs, such as a fast heart rate and/or fast respiratory rate
- The baby has a low level of oxygen in her blood, despite the healthcare team giving extra (“supplemental”) oxygen to the baby
- **Please note that with some congenital heart defects, pulse oximetry may show a normal level of oxygen in the blood, but, in fact, the baby is not getting enough oxygen to vital organs due to blood flow problems.
Below are some signs that a baby is struggling to breathe and may be about to suffer respiratory failure – or may already be in respiratory failure.
- The baby is having retractions, which is typically when, instead of the chest expanding when the child takes a breath, the chest sinks in. Parents (and the healthcare team) can easily see this sign. Types of retractions are:
- Intercostal retractions – these occur between each rib
- Subcostal retractions – when the belly pulls in beneath the rib cage
- Substernal retractions – when the belly pulls beneath the breastbone.
- Other types of retractions include suprasternal retractions, which is when the skin in the middle of the neck sucks in, and supraclavicalular retractions, which occur on the part of the neck above the collarbone.
- The baby’s nostrils are flaring (the nostrils are widening).
- The baby is experiencing stridor, which is wheezing heard on inspiration.
- The baby is using accessory muscles to breathe. The main inspiratory muscles include the diaphragm and the external intercostal and scalene muscles. If the baby is using the sternocleidomastoid (muscles in neck), pectoralis major and minor (muscles in chest), serratus anterior (muscles on the side of the chest), latissimus dorsi (muscle in the back), and serratus posterior superior muscles (muscles at the top of the back, below the neck, and in the lower back, underneath the rib cage), she is using accessory muscles. A baby starts to use accessory muscles as a way to increase ventilation. Once these muscles start being used, the baby will become fatigued very easily and will go into respiratory failure, if she is not already in respiratory failure.
HELP FOR CHILDREN WHO HAVE A BRAIN INJURY CAUSED BY OXYGEN DEPRIVATION

If you think your baby experienced a traumatic birth, oxygen deprivation, a brain bleed, delayed delivery, or delayed emergency C-section, or if your baby’s care was mismanaged after birth in the NICU, please contact our team of experienced Michigan birth injury attorneys. The medical malpractice team at Grewal Law is comprised of attorneys and healthcare professionals, including an on-site registered nurse, pharmacist, paramedic, and respiratory therapist. We also work with the best consultants from around the country, as well as a physician who has an office out our Okemos location.
If your baby was diagnosed with HIE, seizures, cerebral palsy, motor disorders, periventricular leukomalacia (PVL), hydrocephalus, intellectual disabilities, or developmental delays, or if you experienced problems during delivery or shortly before or after birth, please call us. Our medical malpractice attorneys and medical staff are available to speak with you 24/7.









